Case Name: Lost Stent
eJury Case Number: 0062
eJuror: John Smith
eJuror pay: $10.00
Case Type: Mock Jury
Please read the following FACTS very closely, then answer the JURY QUESTIONS, PERSONAL QUESTIONS, and provide any ADDITIONAL COMMENTS. When finished, click the "Submit Verdict" button at the bottom.
FACTS
General Background:
Harold is a 73-year-old male who lives at home with his wife, Lisa. Due to the events which will be described below, he now lives a very sedentary life. He weighs only 160 pounds. He cannot climb stairs, have intimate relations with his wife, or do anything which would make his heart race. He no longer drives a car. He should not go outside if it is hotter than 80degreesor colder than 60 degrees. He has a persistent wet cough. He looks slightly disfigured because his head is permanently locked to his right.He experiences periods of forgetfulness and confusion.
Prior to the events made the basis of this lawsuit, Harold was a relatively healthy man for his age. He was 5', 11" tall and weighed 184 lbs. Other than occasional arthritis in his knees, he was fully functional. He retired after a long career with a large electric company in 1992.
In 1989, when Harold was 62-years-old, he experienced some chest pain, so he went to see Dr. Jones, a local cardiologist. Dr. Jones performed a test called a cardiac catheterization which showed that some of Harold's blood vessels had become clogged and several of his arteries had narrowed due to the formation of plaque. Harold changed his diet, began an exercise program, and started taking medication to lower his cholesterol. He saw Dr. Jones every year for a check-up and stress test. His condition improved over the years, and Dr. Jones even complimented him for being a very good patient.
In September of 1998, Harold underwent a stress test, and based on those results, Dr. Jones recommended that Harold should have another cardiac catheterization test and possibly an angioplasty. Harold went to Metro Hospital on October 20, 1998, to complete the necessary paperwork. He signed a "Disclosure and Consent to Medical Surgical Procedures" form. The form listed both the cardiac catheterization and the angioplasty as the procedures Harold was consenting to. The form had a long list of risks and hazards, including everything from "injury to artery" to "death".
Harold returned to Metro Hospital the following day, October 21, 1998, for the cardiac catheterization test. Although Harold and Lisa arrived in the morning, Dr. Jones' schedule prevented him from doing the test until late in the afternoon. Harold's test was the last test performed that day, and by the time the results were ready, Harold was sound asleep due to medication which had been administered to relax him throughout the day in preparation for the test. So, Dr. Jones reviewed the results with Lisa and Craig (Harold and Lisa's adult son). Dr. Jones showed them an angiogram of Harold's heart and explained that it showed a blockage in one of Harold's arteries. He said the angioplasty would indeed be necessary in order to remove the blockage and increase the blood flow through the artery. Dr. Jones described the angioplasty as a procedure that would use a catheter and a wire with a balloon on the end that he could inflate and deflate as he passed it through Harold's artery. The printed material furnished by Metro Hospital said that the angioplasty would take only one (1) to two (2) hours and that the patient would be awake during the procedure. Dr. Jones suggested to Lisa that they check Harold into a room for the night and do the angioplasty the next day.
The illustration below should give you an idea of how the balloon is inflated to compress the plaque on the inside walls of the artery in a typical angioplasty procedure:
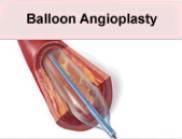
The following day, October 22, 1998, Dr. Jones (who is not an employee of Metro Hospital) began the angioplasty slightly after 1:00 p.m. in a section of the hospital known as the Cath Lab, with a team of hospital nurses and technicians assisting (who are all employees of Metro Hospital). What happened in the next 4 hours and 50 minutes is disputed and is the subject of this lawsuit. What is known for sure is that at 5:50 p.m. Harold went into emergency open-heart surgery. Thanks to the efforts of a thoracic surgeon named Dr. Brown, and the entire open-heart surgery team, Harold's life was saved. Unfortunately, however, their efforts came too late to prevent the damages that have permanently changed Harold's life.
Facts from the Plaintiffs' Perspective:
The angioplasty required Dr. Jones to insert a long, thin tube into the groin area of Harold's leg and pass a guide wire through the tube to position a balloon at the narrow part of Harold's artery in his heart. The medical records confirm the times of the following events:
At 1:15 p.m., the first guide wire could not be passed through the narrow part of Harold's artery. Dr. Jones continued to work on Harold with new wires, but by 1:30 p.m., both a second wire and a third wire had been unsuccessful in getting through the clogged part of Harold's artery. A monitor nurse in the room has testified by deposition that when the third wire failed, she knew this was going to be a difficult procedure. By 2:00 p.m., Dr. Jones had tried a fourth wire, and still no penetration of the clogged artery. Finally at 2:07 p.m., the fifth wire was successfully passed through the narrow opening, and Dr. Jones turned his attention to placing a balloon in the narrow opening to inflate and compress the plaque on the inside of Harold's artery. The balloon was inflated three times, with the third inflation completed at 2:20 p.m., and blood flow improved immediately.
Without talking to Harold, Lisa or Craig, Dr. Jones decided to attempt another procedure on Harold. He took a wire equipped with a device called a stent and tried to advance the wire and the stent into Harold's heart and place the stent permanently inside Harold's clogged artery at the narrow opening. A stent is a very small tube-shaped metal mesh. It is designed to act as a support or brace for the walls of a patient's artery. The stent is intended to hold back the walls and allow the blood to flow through less obstructed. The illustration below shows how the balloon is inflated to press the stent into place:
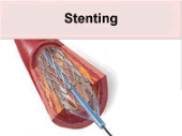
The hospital records show that the stent reached the narrow part of Harold's artery at 2:33 p.m., and Dr. Jones attempted to deploy it. For some reason, Dr. Jones could not position the stent where he wanted, and at 2:52, p.m., he attempted to withdraw the wire and stent. When he pulled out the wire, the stent was missing. Harold's blood pressure dropped sharply, and Dr. Jones says that he put out a call at that time for a surgeon qualified to perform emergency open-heart surgery. However, no surgeon was then available, and no operating room was available.
Harold remained in the Cath Lab and, at 3:24 p.m., Dr. Jones passed into Harold's heart a new wire with a balloon, in an attempt to retrieve the stent by inflating a balloon inside the stent. This effort failed, and Harold's blood pressure dropped sharply again. At 3:39 p.m., Dr. Jones attempted a microsnare (i.e., a tiny hook) on the end of a wire to retrieve the stent, without success. Dr. Jones has testified by deposition that he's never done a procedure before where he "lost" a stent. Finally at 3:48 p.m., Dr. Jones put another balloon into Harold and tried to crush the stent, thinking that if he couldn't get it out, at least he could collapse it or smash it into as small an obstacle as possible and against the wall of the vessel. This effort sent Harold's blood pressure down for the third time, and Harold became severely unstable with a blood pressure of 75/30 at 4:30 p.m. Medications were promptly administered to Harold, and his blood pressure improved by 5:10 p.m., to 140/50. Hospital personnel and Dr. Jones continued to care for Harold, but there was little they could do until the open-heart surgery team was in place and an operating room was available. Harold went slowly down hill, until he was sent to surgery at 5:50 p.m. with a blood pressure of 60/30.
The open-heart surgery team performed a bypass that saved Harold's life, but the next 110 days at Metro Hospital proved very difficult. Lisa stayed with Harold 14 to 16 hours per day. She has lost all trust in doctors and says she was fearful to let Harold out of her sight for even a minute. Harold was eventually moved to a rehab facility and stayed another 53 days, with Lisa being with him most of the time. Harold left the rehab hospital weighing 130 lbs. (having lost 54 lbs.). He had to be taught how to feed himself, talk, bathe, and walk again. Harold's medical bills for his emergency open-heart surgery, hospital stay, rehab, and therapy, total $740,000.00.
A cardiologist expert witness has reviewed Harold's medical file. He says that Harold's October 21, 1998 cardiac catheterization showed very tortuous and calcified (damaged) vessels and arterial blockage that made Harold a very high-risk patient, and Dr. Jones should have recognized this. He believes that Dr. Jones should never have attempted to place a stent through these damaged vessels without ever checking to see if bypass surgery could be immediately performed, if it was needed.
The cardiologist expert, along with a nursing expert, notes that Metro Hospital had a written policy that required the hospital staff to discuss with Dr. Jones the level of stand-by services needed for each patient and to document that level in the chart. The hospital did not do that. Consequently, when Dr. Jones admitted that surgery was needed at 2:52 p.m., a team could not be assembled, and surgery could not be performed until 5:50 p.m. -- three hours later. By then, Harold had become unstable, he had been pumped with heart-altering drugs, and he had begun to lose consciousness. The cardiologist expert believes that the Cath Lab team and Dr. Jones failed to carry out inter-hospital notification to the operating room as soon as the emergency developed. Furthermore, he believes Dr. Jones' attempted crushing of the stent was so bizarre, that the Cath Lab team should have immediately used the hospital's chain of command policy to report what was happening to their supervisors. Crushing is not a medically recognized method of stent retrieval, deployment or salvage, and probably caused Harold to crash (extreme drop in blood pressure that occurred at 4:30 p.m.). The cardiologist expert also points out that the medical records show Harold was taken to surgery in a very unstable condition, which contributed to Harold's many permanent injuries. He believes that Dr. Jones' opinion that the injuries are the result of a blood clot forming after the surgery is just not supported by the records. Harold was at great risk for developing clots because of the extreme delay in the Cath Lab, which would have been unnecessary if Dr. Jones and the hospital's Cath Lab nurses had simply followed policy and made efforts to have bypass surgery on stand-by if needed.
Harold and Lisa asked an expert in physical medicine and rehabilitation to explain to them how Dr. Jones' conduct related to Harold's subsequent problems. He will testify that Harold suffered heart damage, brain injury, and respiratory failure as a result of his experience in the Cath Lab. This expert will also testify that all of Harold's medical complications that followed the dislodgment of the stent are linked to the loss of blood pressure between 2:52 p.m. and 5:50 p.m. The medical bills Harold has incurred related solely to these complications total $740,000. In addition, he thinks Harold will incur additional medical bills in the future ranging from $1,000 to $5,000 per year, to treat the brain, heart and respiratory problems caused by substandard medical care.
Harold and Lisa wanted to know why they received no information about stent placement, so they consulted a nurse with 20 years' experience. She told them that, if Dr. Jones had not discussed the stent with them, hospital admission nurses should have explained the procedure or contacted Dr. Jones' office, to make sure that Harold and Lisa knew the extent of the procedure that might be used. Harold and Lisa also wanted to know more about Metro Hospital's responsibility to make sure that Harold received good nursing care and a prompt transfer to emergency surgery. They consulted a nurse who is a registered cardiovascular invasive specialist with 15 years in the Cath Lab and over 10,090 cases completed. He points out, as does the cardiologist, that the hospital's Cath Lab personnel never verified whether bypass surgery might be needed, did not discuss that need with Dr. Jones, Harold or his family, and did not document any such need for the other hospital personnel to reference. Consequently, this procedure, which was a high risk for stent failure and a high risk for needing bypass surgery, was performed when no bypass surgery was available ' in direct violation of the hospital's policy. The result was a three-hour wait, while Harold was deprived of precious blood and oxygen to his brain. He faults Metro Hospital's nursing team in two areas: (1) they failed to follow hospital policy, designed to prevent this specific tragedy; (2) they failed to use their efforts to get an operating room staff ready to assist with Harold's care. Harold and Lisa's team of experts acknowledge that Metro Hospital does not practice medicine, but that Metro is required to have nurses in the Cath Lab sufficiently trained to recognize that Harold was at high risk of this procedure failing and they should have politely discussed this with Dr. Jones. They also acknowledge that patients have a duty to be cautious; however, they trusted Dr. Jones to tell them if they should get other opinions. He did not, and he has admitted he did not. Harold and Lisa would never have consented to this procedure if they had known there would be an attempted stenting and that no surgeon was available if the procedure failed. The "Disclosure and Consent to Medical Surgical Procedures" form signed by Harold 2 days before the procedure does not mention stenting.
Facts from Defendant Dr. Jones' Perspective:
I have cared for Harold as his cardiologist for more than ten (10) years. Harold had a catheterization in 1989 and the test showed several areas of damaged arteries. In 1998, he was not in good health and could not perform a treadmill stress test, due to bad knees. A chemical test indicated further blockage, so I asked my nurse to schedule Harold for another catheterization. I knew Harold had been through this procedure before, so I expected that he would ask me if he had any questions or concerns. He did not have any. The catheterization was performed without problems, and I was able to determine that many of the blockages were old blockages that had not changed over the last ten years. There was one blockage, however, that appeared to be an active blockage. Since there was only one problem blockage, it was my decision that Harold was not a candidate for bypass surgery, and I concluded the appropriate treatment was to do a balloon angioplasty on the problem area, then place a stent there to keep the a artery open. After the catheterization, I showed Lisa a picture of the blockage that I wanted to try to open and relieve. I explained that it might prove difficult to reach and, if I couldn't reach the lesion and place the stent where the blockage was, we would have to convert to bypass surgery. Lisa listened and understood what I was going to do. I began the balloon angioplasty and attempted stent placement procedures about 1:00 p.m. on 10/22. The lesion did prove difficult to reach, but I managed to inflate the balloon over the lesion and improve circulation from approximately 2% to 40%. This was not enough improvement, in my judgment, so I proceeded to place the stent at the site of the blockage. Unfortunately, the stent was knocked off its delivery balloon by plaque and calcium deposits on the wall of the arteries leading to the lesion (the blocked area). I did not expect to lose the stent and tried to avoid that happening. However, this is always a risk, and it was a risk in this case, but the stent has to be passed across these rough areas to get to where the blockage is located. There is no other way to get the stent to the blockage. I was slow and deliberate and careful, but the stent was knocked from the balloon. I tried several different methods to retrieve the stent but could not get it back out of the heart, so bypass surgery was the only option. Harold remained relatively stable during the entire procedure, but his blood pressure began to fall near the end of the procedure. When I learned the stent was lost, I knew that surgery was necessary, but at that time, unfortunately, there was no operating room available at the hospital and no thoracic surgeon available. So I kept the patient comfortable until an operating room and surgical team were available. Harold was taken to surgery as soon as we could get him there. At one point, I even crushed the lodged stent into the wall of the artery to assure adequate blood flow.
I am sorry there wasn't an operating room available the minute we needed one, but that can and does sometimes happen in hospitals. That is no one's fault. There are just so many operating rooms, and just so many thoracic surgeons in an area.
Whether or not the arteries have severe plaque build up, or the vessels are very crooked and hard to get through, it is obvious there are risks inherent in the procedure that the stent may be dislodged. But the probability that the stent will be lost or dislodged is very low, and the failure to open the artery could cause the patient's death. Stenting, if successful, is much less painful, much less invasive, much less expensive, and the patient recovers more rapidly. Harold and Lisa claim that I did not tell them I might attempt to place a stent in the artery. That is not correct. Unfortunately, they do not recall that conversation with me. If they had questions or concerns, or if they wanted another cardiologist's opinion, I would expect them to ask me. They did not. I believe I provided adequate explanation of the procedures I was going to do and the risks involved. There are serious risks anytime the procedure requires entering the heart. No procedure is ever risk free. Certainly, Harold and Lisa knew this. There were also serious consequences if I stood by and did nothing. What I did was in the patient's best interest. It is very unfortunate that Harold developed any complications following the bypass surgery. But those complications resulted from a clot that developed after the bypass surgery, and is a known risk following bypass surgery. I had nothing to do with this complication.
I have also had Harold's medical records reviewed by a cardiologist expert witness. He thinks that Harold's longstanding history of coronary artery disease created circumstances supporting my effort to get more blood to Harold's heart by the least complicated method, which was angioplasty and stenting. He feels that single vessel disease such as Harold's should always be treated in the most conservative manner possible. The most conservative method is usually the best method for a man in Harold's age bracket.
Facts from Defendant Metro Hospital's Perspective:
Metro Hospital is thankful that Harold has significantly recovered and has returned to most of his normal daily activities. Unfortunately, Metro Hospital cannot guarantee that the doctors using their facility will never encounter complications that require extended care. Harold and Lisa were given plenty of time to ask questions about the angioplasty, and they signed all of the forms indicating that they understood the planned procedures. The nursing staff provides assistance, and only assistance, to cardiologists in the Cath Lab. The Cath Lab nurses made no decisions concerning the best manner to get more blood to Harold's heart, and none of them were qualified to question the appropriateness of Dr. Jones' efforts to retrieve the stent. Metro Hospital is proud of the job that their nurses did in getting Harold to the emergency open-heart surgery team, and by everyone working together, Harold's life was saved. Metro's policy to document the level of stand-by services needed would not have changed the outcome of Harold's case. Dr. Jones was the only person qualified to make that determination, and he did not do so.
The hospital provided nurses to assist Dr. Jones, not to tell him what to do as a physician. These nurses are not licensed to practice medicine. Patients admitted to the hospital want the nurses to provide nursing care, not make medical decisions. This hospital has excellent facilities, but it has only two operating rooms to perform bypass surgery. When our nurses were told that surgery was needed, they moved quickly and appropriately to get the operating room ready for the patient. We cannot keep an operating room and surgical team available and on call for every angioplasty. We will get it ready when the cardiologist tells us to, and that is what we did. Cath lab nurses cannot practice medicine.
JURY QUESTIONS
The following definitions, instructions, and questions are derived from the Texas Pattern Jury Charges. The following is the exact same language the actual jury will receive if this case goes to trial. Each instruction, though appearing redundant at times, is important. Some of the definitions and questions are very difficult, and unfortunately, it is very rare that a Judge would ever allow them to be modified. Answer to the best of your ability. If you have particular difficulty, you can explain the difficulty in your answer.
DEFINITIONS
Negligence: when used with respect to the conduct of Dr. Jones, means failure to use ordinary care, that is, failing to do that which a cardiologist of ordinary prudence would have done under the same or similar circumstances or doing that which a cardiologist of ordinary prudence would not have done under the same or similar circumstances.
Ordinary Care: when used with respect to the conduct of Dr. Jones, means that degree of care that a cardiologist of ordinary prudence would be use under the same or similar circumstances.
Proximate Cause: when used with respect to the conduct of Dr. Jones, means that cause which, in a natural and continuous sequence, produces an event, and without which cause such event would not have occurred. In order to be a proximate cause, the act or omission complained of must be such that a cardiologist using ordinary care would have foreseen that the event, or some similar event, might reasonably result therefrom. There may be more than one proximate cause of an event.
Negligence: when used with respect to the conduct of Metro Hospital, means failure to use ordinary care, that is, failing to do that which a hospital of ordinary prudence would have done under the same or similar circumstances or doing that which a hospital of ordinary prudence would not have done under the same or similar circumstances.
Ordinary Care: when used with respect to the conduct of Metro Hospital, means that degree of care that a hospital of ordinary prudence would be use under the same or similar circumstances.
Proximate Cause: when used with respect to the conduct of Metro Hospital, means that cause which, in a natural and continuous sequence, produces an event, and without which cause such event would not have occurred. In order to be a proximate cause, the act or omission complained of must be such that a hospital using ordinary care would have foreseen that the event, or some similar event, might reasonably result therefrom. There may be more than one proximate cause of an event.